CSF Leak Canada
October 10, 2025Hi Everyone!
I'm so sorry for being MIA for the last few years, I was dealing with a severe heath crisis that took a long time to resolve. From September 2002 to January 2024, I was in a wheelchair and unable to walk due to a severe CSF Leak, I had to advocate and push to be diagnosed then finally be treated at Sunnybrook hospital in Toronto. It was a long and lonely road fighting through a nightmarish health care roadblock. I was going from hospital to hospital, doctor to doctor, begging for help and turned away quickly by many doctors saying that they "didn't have enough resources or skilled doctors to help me".
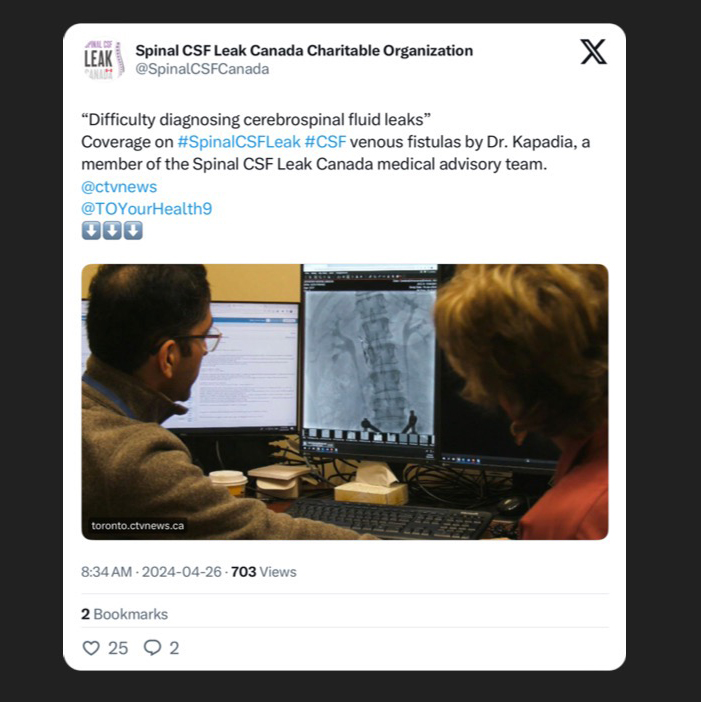
I thought to myself that this should not be happening in Canada. After spending months in a local hospital, I finally had enough and reached out to the news media for assistance in raising more awareness about the lack of education regarding CSF Leaks in Canada, particularly amongst doctors.
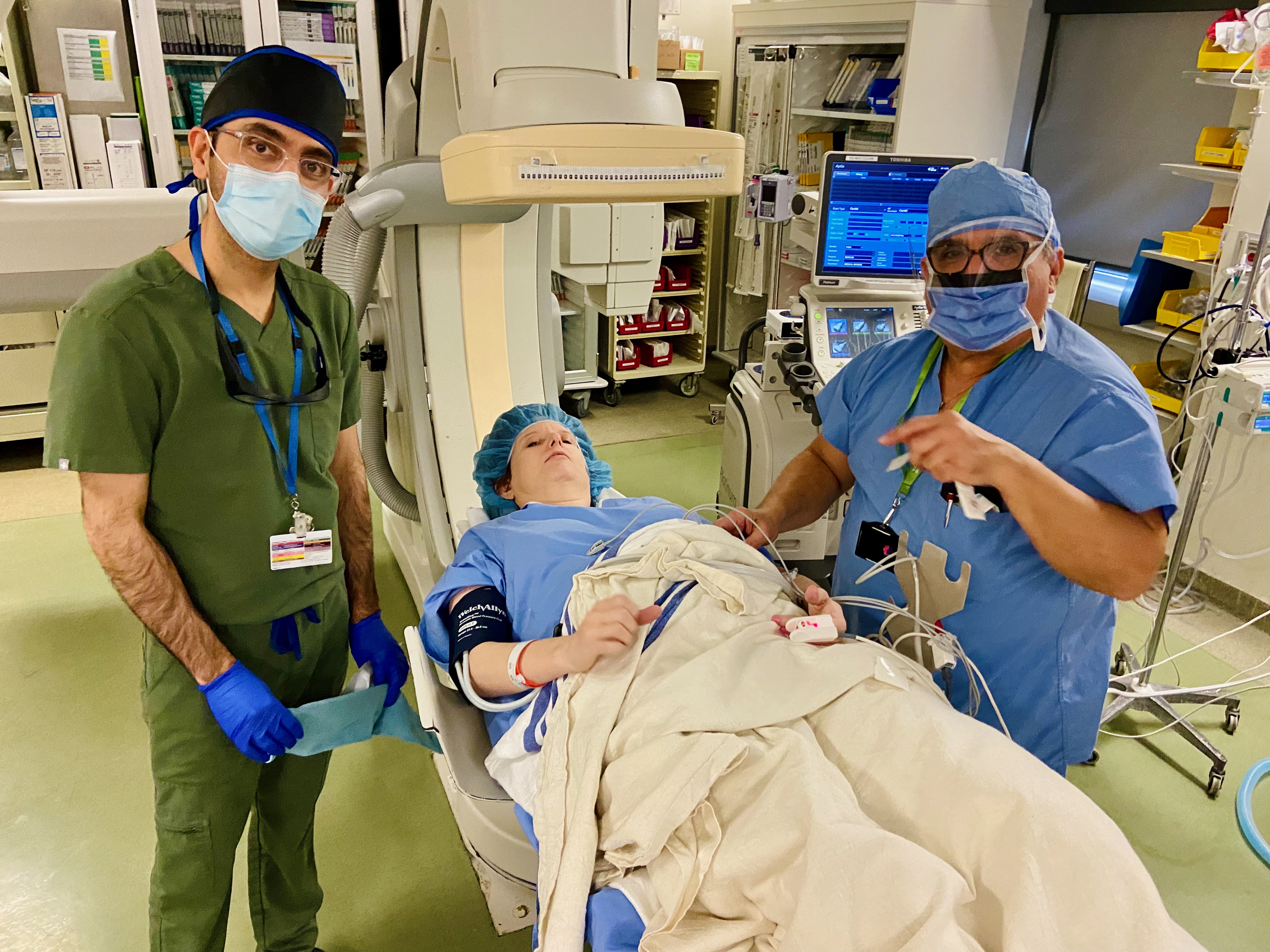
When I connected with CTV News, I was about to undergo surgery to get my CSF Leak sealed and they agreed to do a story on me so that we can help so many others in Canada. Once the story was aired all across Canada, I was overwhelmed with messages from so many patients who were equally as desperate as me to be diagnosed and treated in a timely manner. My doctor and I were thrilled with the overwhelming success, he is now widely recognized for his talent and expertise at detecting a very difficult spinal disorder. He trained at one of the top CSF Leak clinics in the US, and is one of the very few doctors in North America helping patients with this debilitating disorder. He is now in high demand with patients coming to Sunnybrook from coast to coast.
.jpeg)
Unfortunately, many patients don't know where to go or who to ask for help. Our Canadian support group has over 600 patients which continues to grow every month. Our small non-profit group, CSF Leak Canada, wants to help them and so do I. They want to feature my story on their website but CTV News has made that task nearly impossible. Their fee is astronomical, they are charging $20 per SECOND to use my video, if we want to use 60 seconds featuring my doctor and myself at Sunnybrook hospital, it will cost us $1200 or more, for 3 minutes it will cost us over $3000.
I personally cannot afford this, nor can our small organization. Our goal is to reach as many patients as possible and to stop some of them from dying, we have lost several of our dear friends in the last few years since they could not access the treatment they desperately needed and unfortunately had to use MAID. I was going down that road myself and had chosen that option when I stumbled across this wonderful group who helped me find Dr. Kapadia at Sunnybrook. He literally saved my life.
Within days of our story airing on CTV News, I received numerous emails and messages from patients all across Canada asking for help to see Dr. Kapadia at Sunnybrook hospital, he is now in demand with a high rate of success. He is doing phenomenal work with patients suffering from CSF leaks, he is extraordinarily talented and very compassionate. He was the first doctor to really listen and believe in me. I am incredibly grateful that I found him.
He is helping so many of us regain a normal life again. Dr Kapadia recently received an award which recognized his hard work, dedication, commitment and compassion towards all of us, he is truly a remarkable doctor. Sunnybrook will be dedicating a wing for his CSF Leak team to use since he is so popular now and his practice has grown considerably.
I am currently looking into possible grants from the government, however, I am not having much luck and running out of time. You can help us make this dream possible by donating to CSF Leak Canada so that we can make a difference. Please include a note stating that you would like to use the donation for “Jennifer’s CTV News footage”.
The donation can be made directly to Spinal CSF Leak Canada through our website https://www.spinalcsfleakcanada.ca/donate.
Thank you so much from the bottom of my heart, every dollar counts! I will be donating some of my CSF Leak art so that we can sell shirts and various items on our website once the store is up and running.
Posted by jennifer gibson. Posted In : 2025